August 13, 2021 | Jessica Zeff
3 Minute Read
Headlines From the FY 2022 SNF PPS Final Rule
CMS released the FY 2022 Skilled Nursing Facility (SNF) Prospective Payment System (PPS) Final Rule on July 29, 2021 and there were no real surprises for those of us familiar with the 2022 proposed rule.
Key Takeaways
- The final rule confirmed payment updates for skilled nursing facilities which will result in an estimated $410 million increase in payments compared to last year.
- No changes were made to the Patient Driven Payment Model (PDPM) structure, however, CMS noted that a recalibration of the PDPM Parity Adjustment is forthcoming, and stakeholders will need to look to future rulemaking to see how CMS plans to recoup the 5% increase in spending they have seen since implementing PDPM.
- Slight changes are being made to the quality programs for SNFs. CMS continues to gather information on expanding the programs and making them interoperable by using digital quality measures (dQMs) and Fast Healthcare Interoperability Resources (FHIR).
The changes in this final rule will be effective on October 1, 2021.
Market Basket Update
The market basket rate update has been set at 2.7% for FY 2022. This increases payment by 1.2%, and results in an estimated increase of $410 million for Medicare Part A payments to SNFs compared to FY 2021. The 1.2% increase includes the 0.8% forecast error adjustment and the 0.7% productivity adjustment that are subtracted from the market basket percentage.
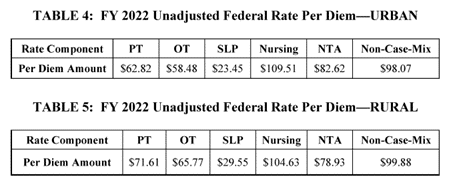
Unadjusted Federal Per Diem Rates
Unadjusted federal rates for FY 2022 are:
Case-Mix Adjustment
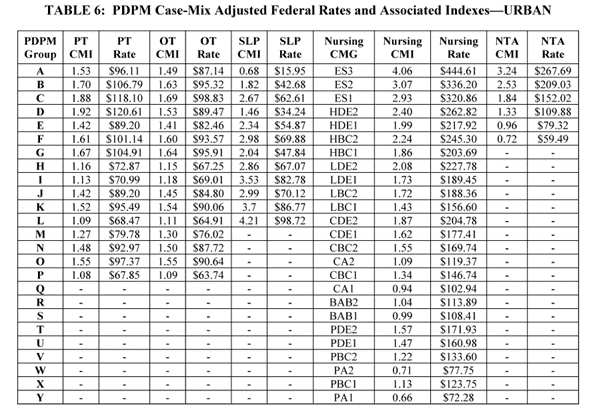
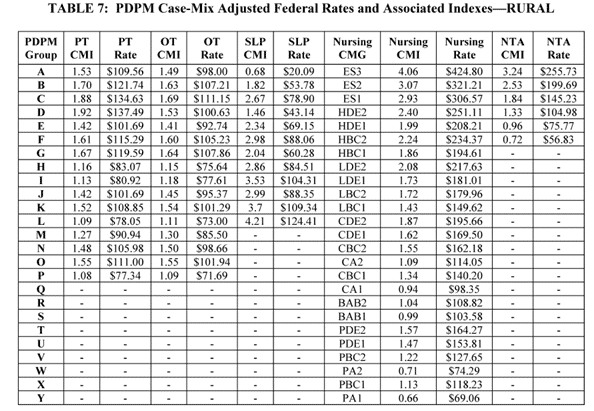
Final FY 2022 Case-Mix Rates are outlined in the tables below. These tables do not reflect the adjustments that may be made related to the SNF Value-Based Purchasing Program. (The SNF VBP Program is a CMS program that provides SNFs with incentive payments based on the quality of care they provide, as measured by performance on a measure of hospital readmissions.)
Wage Index
CMS has finalized the adoption of the OMB 20-01 geographic delineations for FY 2022 but reiterates that the updated version does not change the OMB 18-04 updates that were adopted last year. The FY 2021 SNF PPS Final Rule allowed for a 1-year transition policy inclusive of a 5% cap on reductions in the wage index due to core based statistical area (CBSA) reclassification of urban and rural counties. This policy was not modified or extended in this final rule, so changes to the wage index will be completed in FY 2022.
Wage index tables for FY 2022 are available on the CMS website. See link in Resources section.
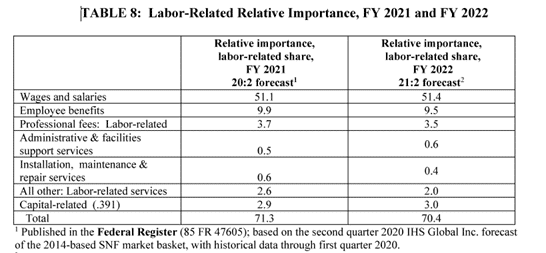
Labor-Related Share
For FY 2022, the labor-related share component of the diagnosis-related groups (DRGs) was updated to reflect the 2018-based SNF market basket. This resulted in a decrease of 0.9% from FY 2021. It has been finalized as 70.4% for FY 2022.
Consolidated Billing
Certain blood clotting factors (BCFs) used for the treatment of hemophilia and other bleeding disorders, as identified by HCPCS codes, have been finalized to be excluded from consolidated billing for SNFs. Additional HCPCS codes not included in the proposed rule were added to the list. These are separately billable under Part B when furnished to a SNF’s Part A resident. Due to the unbundling of services, CMS has finalized a $0.02 in the unadjusted urban and rural rates to reflect the exclusion of BCFs.
CMS is also adding another chemotherapy drug: RIABNI to the list of excluded codes.
A list of excluded codes is available on the SNF Consolidated Billing website. See Resources section for link.
Administrative Presumption
There are no changes to Administrative Presumption for FY 2022.
Patient Driven Payment Model (PDPM)
PDPM ICD-10 Mapping Updates
Several changes to mappings were finalized as proposed, and are outlined in the table below:
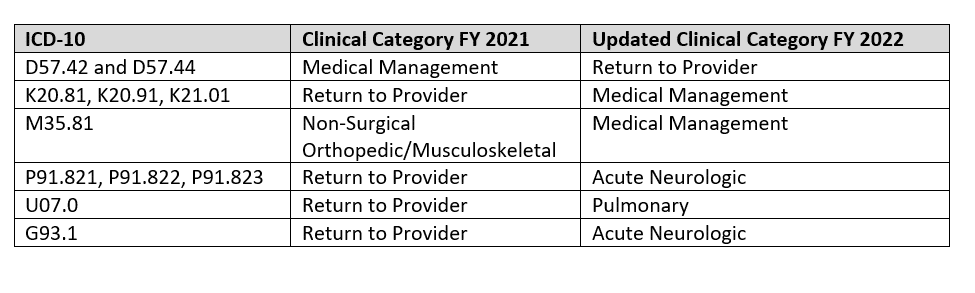

PDPM Mapping files can be found on the PDPM website and a link can be found at the bottom of this article.
PDPM Parity Adjustment
CMS noted a significant increase in overall payment levels under the SNF PPS and they believe a recalibration of the PDPM parity adjustment is needed. Action to recalibrate will be taken in future rulemaking to adjust for the approximate 5% increase in payments that have been made since moving to PDPM from RUGs IV. No changes were finalized for FY 2022, but CMS intends to have additional information on proposed methods to recalibrate the PDPM Parity Adjustment in the FY 2023 SNF PPS Proposed Rule.
MDS Updates
No changes to the MDS were noted in this final rule. As a reminder, CMS stated in the May 8, 2020, IFC, that the MDS updates will be implemented no sooner than the October 1 date that is at least two full fiscal years after the COVID-19 PHE ends.
SNF Quality Reporting Program (QRP)
SNFs that do not meet reporting requirements of the QRP will be subject to a 2% reduction in their annual update.
For FY 2022, there are 13 Quality Measures adopted for use. See Table 24 in the Final Rule for details.
CMS finalized the addition of two new measures for the FY 2023 QRP:
- Skilled Nursing Facility (SNF) Healthcare-Associated Infections (HAI) Requiring Hospitalization Measure. This is a claims-based measure so no additional data will be required from SNFs.
- COVID-19 Vaccination Coverage Among Healthcare Personnel (HCP) Measure. To comply with FY 2023 reporting, this measure would require vaccination data submission to the CDC/NHSN (National Healthcare Safety Network) beginning 10/1/2021-12/31/2021 for the first quarter. SNFs will be required to submit data for the entire calendar year beginning FY 2024. Reporting must take place one week out of each month.
CMS finalized an update to the following measure for FY 2023 reporting period:
- Transfer of Health (TOH) Information to the Patient – Post-Acute Care (PAC) Measure. The denominator will be updated to exclude residents discharged home under the care of an organized home health service or hospice. This aligns with the IRF, HH and LTCH QRPs.
COVID-19 Affected Reporting (CAR): The rule finalized the use of limited data for quality reporting in the SNF QRP program. This means that data affected by the PHE will be excluded from calculations. This method allows for a data refresh in January 2022 for updated public reporting and will continue with limited data through July 2023.
SNF Value-Based Purchasing (VBP) Program
CMS has finalized a policy to suppress the Skilled Nursing Facility 30-Day All-Cause Readmission Measure (SNFRM) for the FY 2022 VBP Program. All participating SNFs will receive a performance score of zero regardless of performance. CMS is required to withhold 2% from the federal adjusted per diem rates for participants and will be awarding back 60% of that to all SNFs in the VBP programs. An incentive payment of 1.2% for all participating SNFs will be given. Those receiving a low volume adjustment would receive the full 2% payback.
For FY 2023, CMS is adjusting the lookback period of the SNFRM to include only FY 2021 data (90 days) due to the PHE.
Other
Digital Quality Measures (dQMs)
CMS asked for comments on the future adoption of dQMs. It will use the feedback received for policy development in the future.
Disclaimer:
The information contained in this article is a summary and intended for educational purposes only. Interpretation of final rules and any guidance should be reviewed with your legal and compliance teams for applicability to your practice or organization.
References:
FY 2022 SNF PPS Final Rule Fact Sheet
FY 2022 SNF PPS Final Rule (published 8/4/2021)
SNF Value-Based Purchasing Program





