May 5, 2022 | Net Health
3 Minute Read
Remote Therapeutic Monitoring Codes: What’s New in 2022?
It seems nowadays, and I’m sure you’ll sympathize, there’s something new on the healthcare horizon every time I turn around. I know this is par for the course and it’s also why I find regulatory compliance so exciting.
So, it was in mid-turn around that remote therapeutic monitoring (RTM) found me and my team. (You’d think we’d know not to turn around by now but, like you, we’re clearly gluttons for punishment. I’m kidding – we actually really love what we do!)
What’s The Difference between Remote Therapeutic Monitoring (RTM) & Remote Patient Monitoring(RPM)?
Many of you reading this probably have already heard about Remote Therapeutic Monitoring (RTM). And some of you, if you’re like me, may have initially confused it with remote physiologic monitoring or remote patient monitoring, or any other monitoring involving RPM as an acronym.
“There’s a difference,” you ask? Gotcha! Yes, there is so let’s look at what RTM is and review the guidance CMS recently released in the 2022 Medicare Physician Fee Schedule regarding Remote Therapeutic Monitoring (RTM) services.
Remote therapeutic monitoring (RTM) is, essentially, the use of a medical device (as defined by the Food and Drug Administration) to monitor a patient’s health or response to treatment using non-physiological data.
Remote therapeutic monitoring (RTM) can be used for remote patient monitoring. Things such as medication adherence, response to therapy, musculoskeletal activity, and respiratory activity.
This means that RTM can be used to monitor treatment, for example, specific to pain, functional status, and adherence to exercise therapy. Moreover, Remote Therapeutic Monitoring allows for self-reported data from the patient.
And how is this different from the Rapid Prompting Method (RPM)? The Rapid Prompting Method (RPM) describes non-face-to-face monitoring and analysis of physiologic factors used to understand a patient’s health status.
For example, monitoring of blood pressure, blood sugar level, heart rate.1 Also, RPM monitoring cannot include patient reported data, that is, any data has to be digitally (i.e., automatically) uploaded to the provider (i.e., data cannot be self-recorded or self-reported by the patient).2
Understanding the RTM Codes
Ok, we’re on the same page now and we understand the difference between Remote Therapeutic Monitoring (RTM) and Rapid Promoting Method (RPM). You’d probably like to know what the codes are and how to use them, so let’s dive in!
First, let’s start with the codes.
There are 5 new codes for RTM services as of last year. Effective January 1, 2022, health care providers can use these codes to remotely monitor and review data related to signs, symptoms, and functions of a therapeutic response.
Using definitions from the American Medical Association, we created a handy guide to the 5 new codes.
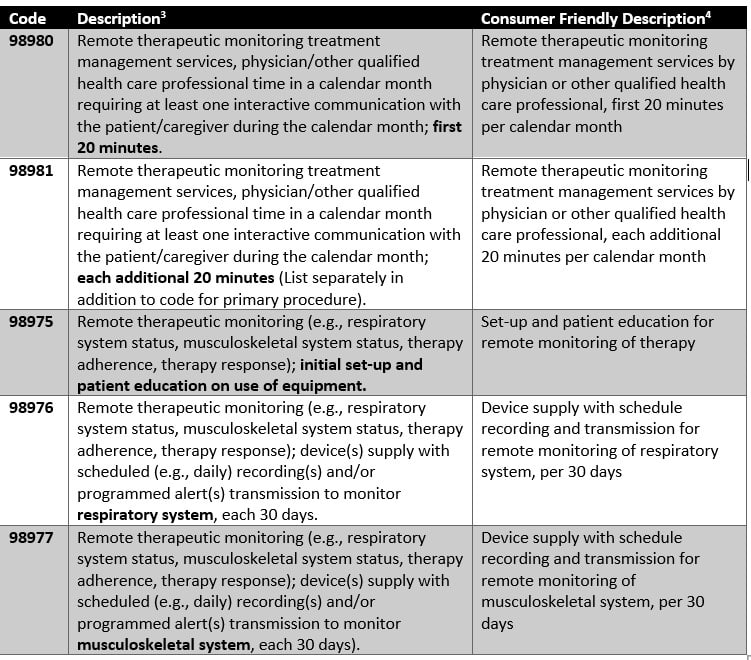
Second, RTM codes can be separated into two subsections:
- 1) Remote Therapeutic Monitoring; and
- 2) Remote Therapeutic Monitoring Treatment Management Services.
Remote Therapeutic Monitoring codes (98975, 98976, 98977) generally describe initial setup, patient education, and device supply. The two RTM Treatment Management service codes (98980 and 98981) are meant to be used to report the time the clinician spends managing the RTM treatment.
Finally, each set of codes has specific guidelines that must be considered before providing and billing for these services. While the details of these guidelines are beyond the scope of this blog, I strongly urge you to make sure you understand these guidelines before implementing Remote Therapeutic Monitoring.
Billing Codes 98980 & 98981
And because nothing about billing is ever straightforward, it might help you to understand the following about these two codes:
- The time spent should be reported per calendar month.
- Time spent does not include clinical staff time required for data collection.
- At least one interactive communication with the patient or caregiver must take place during the calendar month to bill these codes. This interaction contributes to the total time and does not necessarily represent the cumulative time of the service.
- At least 20 minutes of cumulative time must be completed before reporting 98980 for a calendar month. A full 20 minutes must be reached before billing this code.
- Report 98981 for each additional 20 minutes completed in the calendar month. A full 20 minutes must be reached before billing this code.
Defining a Medical Device
You’re still here? Great because we’re not quite done with Remote Therapeutic Monitoring (RPM) codes yet! Thus far we’ve been talking about what the new RTM codes are and clarified some not so clear points about billing. What we haven’t really looked at yet is the meaning of a “medical device” – and understanding the definition of a medical device is key if you’re going to use an RTM code.
I will warn you now, though, that the definition of a medical device isn’t particularly clear and there is no one-size-fits-all method for determining what is or is not a medical device.
My suggestion is to work with your clinical and compliance or legal teams to determine whether the device you intend to use for RTM meets the definition of a medical device.
CPT Assistant Feb 20224 notes that medical devices, as defined by the Food and Drug Administration (FDA), typically capture data using a signal that measures parameters from “within, attached to or external to the body, or captures and electrochemical or photometric response for a medical purpose.” Commercial insurance providers may have different requirements.
The FDA defines a medical device as “an instrument, apparatus, implement, machine, contrivance…or other similar or related article, including a component part, or accessory which is…intended for use in the diagnosis of disease or other conditions, or in the cure, mitigation, treatment, or prevention of disease [or] injury, in man.”5
The FDA further states that software, depending on its functionality, can also be a medical device.6
Remote Therapeutic Monitoring (RTM) Documentation
Note that rehab therapy documentation requirements for RTM have not been defined by CMS or other payers but it’s worth keeping in mind the following may be required:
- Order for service from physician or other qualified health care professional, such as a physical therapist
- Include RTM in plan of care
- Type of device used – name and description o Include musculoskeletal or respiratory device
- Specific education and training provided to the patient and/or caregiver
- Data gathered from the device o Evidence of at least 16 days of monitoring per 30 days
- Date and time of patient and/or caregiver interaction
- Specifics of patient and/or caregiver interaction
- Decisions made that may impact treatment and plan of care
Additional Billing Considerations
- All RTM services must be provided under a therapy plan of care
- These codes are considered “sometimes therapy” codes
- MPPR does not apply to these codes
- These codes do apply to the annual therapy threshold calculations
- Codes 98975, 98980, and 98981 are subject to the de minimis standard if provided by a therapist assistant
- If a patient owns the device used for monitoring, code 98975 should not be billed
Final Words on Remote Therapeutic Monitoring Codes
That’s all I’ve got folks and all I’ve got left to give you just now is a resounding “good luck!” I hope this blog has gone some way to help you understand what the new RTM codes are and how to use them.
Please keep in mind, though, that the information and material in this blog are provided for educational purposes only and is only as accurate as current guidance allows. Readers should consult CMS guidance and their own internal resources to ensure correct billing of any RTM codes.
Note: Net Health makes no representations as to accuracy, completeness, correctness, suitability, or validity of any of the information presented herein. All information is provided on an as-is basis. It is the viewer’s responsibility to verify any and all information presented herein.
References:
1 Foley and Lardner, LLP, “2021 Medicare Remote Patient Monitoring FAQs: CMS Issues Final Rule,” 7 December 2020.
2 Foley and Lardner LLP, “2022 Medicare Remote Therapeutic Monitoring FAQs: CMS Final Rule,” 11 November 2021.
3 The American Medical Association, Current Procedural Terminology CPT 2022 Professional Edition, February 2022.
4 VitalWare Software by HealthCatalyst
5 U.S. Food and Drug Administration, “How To Determine If Your Product is a Medical Device,” 16 December 2019.
6 U.S. Food and Drug Administration, “Policy for Device Software Functions and Mobile Medical Applications. Guidance for Industry and Food and Drug Administration Staff,” 27 September 2019.





